Lung cancer: causes, symptoms, diagnosis and life expectancy – Lung cancer to smoking: the point with Pr. Girard, pneumo-oncologist.
Lung cancer is not uncommon; it is even the third most common cancer in France, with 46,363 new cases recorded in 2018. But beware: ” there is not one lung cancer, but several. It is a very heterogeneous disease “, we immediately warns Pr. Nicolas Girard, pneumo-oncologist at the Institut Curie.
If, as their name suggests, all lung cancers initially develop in the lungs, ” the cancerous tumour itself can originate from different lung cells, resulting in “types” of cancers very precise “, remarks the specialist.
The most frequent lung cancer is non-small cell lung cancer: the malignant tumour then develops thanks to the unchecked multiplication of the epithelium cells. Glandular lung tissue (which is on the outer surface of the lung ) or epithelial lung tissue cells (which line the inside of the lung).
Then comes small cell lung cancer, which develops from the neuroendocrine cells of the bronchi.
Table of Contents
1. Lung Cancer : Smoking Remains The Foremost Risk Factor
To know. Lung cancer affects most men,” although this disease is on the rise in women “, notes Prof. Nicolas Girard. The age at diagnosis is around 67 for men 65 for women. ” Lung cancer is very exceptional in children “, specifies the pneumo-oncologist.
2. What Are The Risk Issues For Lung Cancer?
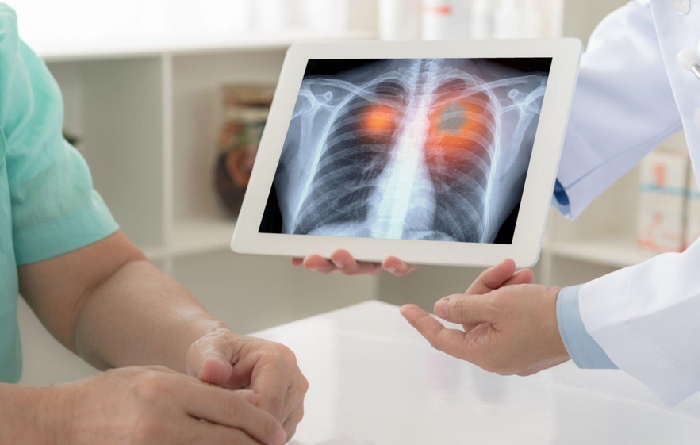
Unsurprisingly, “the” main risk factor for lung cancer is tobacco. ” Smoking is involved in about 80% of cases, and it is the cause of the vast majority of small cell lung cancers “, underlines Prof. Nicolas Girard.
” In smokers, the risk of developing lung cancer increases exponentially and is acquired over time. In other words: quitting smoking “blocks” the progression of the risk but does not allow it to come down “, explains the specialist.
However, in France, 15% of lung cancers occur in non-smokers: ” there are other risk factors which are rarer, in particular occupational exposure to certain heavy metals, asbestos, arsenic.
3. Lung Cancer: It Usually Starts Silently
Unfortunately, lung cancer begins silently in most cases: there are no symptoms. Rarely one can observe the appearance of a chronic cough, sometimes bloody sputum (hemoptysis), difficulty breathing, repeated respiratory infections. Loss of appetite or weight loss. ” In approximately 70% of patients, lung cancer at the metastatic stage, that is to say late, when cancer has spread to organs other than the lungs, ” explains Prof. Nicolas Girard.
In the case of lung cancer, we can thus observe the development of metastases in the brain, liver, bones or even the adrenal glands. “These metastases give symptoms” according to their location “: it can, in particular, be a question of bone pain, convulsive crises, paralysis.
4. Lung Cancer : In France, No Organized Screening
” In France, there is, unfortunately, no organized screening for lung cancer: this is, however, the case in England, the Netherlands, Belgium, Canada and the United States, ” remarks the pneumo-oncologist.
” The French health authorities tend to adhere to this old belief that patients are “responsible” for their lung cancer because they have smoked: however, we now know that smoking is an addiction, therefore a disease ” According to the specialist, this organized screening would, however, reduce lung cancer mortality by approximately 25% in men and 40% in women.
Pr. Nicolas Girard recommends lung cancer screening for people at risk: ” You are at risk if you are over 50 and have smoked for / you have been smoking for over 25 years. ” This screening takes the form of a chest CT scan.
5. Lung Cancer: How It Diagnosed?
The diagnosis of lung cancer takes place in several stages. In addition to the chest scanner, the lung X-ray is useless in the event of lung cancer, “underlines Pr. Nicolas Girard), the doctor will prescribe an extensive assessment to know if there are metastases. These can use a PET scan, possibly supplemented by an MRI of the brain. ” The diagnosis of lung cancer with the help of a biopsy, ” adds the specialist.
6. Lung Cancer: There Are Targeted Treatments
If cancer before the metastatic stage, surgery can be considered: ” concretely, this consists of removing the tumour and supplementing with chemotherapy “, explains the specialist. The risk of relapse is high (approximately 50% within five years), but the survival rate is about 60% – 70% at five years.
” In the case of metastatic lung cancer, genetic testing is essential, ” says Prof. Nicolas Girard. Treatment consists of immunotherapy which will “reactivate” the patient’s immune defences against cancer. This immunotherapy can help with chemotherapy. ”
Warning! ” When a targetable, immunotherapy is unsuccessful: that is the whole point of genetic testing! You have to look for congenital abnormalities to identify them. The health authorities recommend searching for at least four monsters out of the ten most frequent anomalies. Too many patients are still treated with immunotherapy when a targeted treatment could have been possible. ”
-
Lung Cancer: What Is The Life Expectancy?
Lung Cancer – Life Expectancy – The survival rate of lung cancer patients depends on the stage of the disease. ” It is around 30% if the cancer is metastatic and treated by immunotherapy; it is a little higher in the case of targeted treatment “, replies the pneumo-oncologist.
What is Lung Cancer And 10
The lung cancer ICD-10 code is C34. Healthcare practitioners utilise the International Categorization of Diseases, 10th version (ICD-10), a medical categorisation system to categorise and code diagnoses, symptoms, and procedures. The term “C34” refers explicitly to lung and bronchial malignant neoplasms. Although the ICD-10 code for lung cancer may vary based on the precise form and location of the disease, it is crucial to note.
ICD 10 Cases Of Lung Cancer
The classification of illnesses and medical conditions is done using ICD-10 codes. For example, the ICD-10 code for lung cancer is C34. Lung cancer has several causes, including:
Smoking: Lung cancer is primarily brought on by smoking. According to estimates, smoking accounts for 80–90% of lung cancer occurrences.
Secondhand smoke exposure: Lung cancer risk is higher for those frequently exposed to secondary smoke.
Environmental considerations: Exposure to certain environmental variables such as radon, asbestos, and air pollution can raise lung cancer risk.
Family history: A lung cancer gene can make you more likely to get the disease.
Genetic changes: Some genetic differences can make people more likely to have lung cancer.
Age: As people age, their risk of acquiring lung cancer rises.
It is significant to remember that not everyone who gets lung cancer has a known risk factor. Furthermore, a risk factor does not guarantee that a person will get lung cancer.

